Disclaimer: I’ve written this post from my perspective as a mother and a scientist so that others may learn from my decision making process. As part of my research, I spoke with my prenatal care providers to get their medical advice on cord blood donation versus private banking. Given that my child’s family history is entirely free of any disorders that currently benefit from cord blood transplantation, public donation was deemed an appropriate course of action. My care providers and I also discussed the pros (making lifesaving cord blood available to patients who need it) as well as the cons (no prolonged delayed clamping of the umbilical cord) of collecting the cord blood, and we decided together that the pros outweighed the cons. Thus, while I encourage you to do your research and learn what you can about cord blood and its uses, I remind readers that I am not an MD and I do not dispense medical advice. You should take your research and your questions and discuss your individual situation with your care provider to make the decision that is best for you, your baby, and your family.
As an expectant mom, I am bombarded by ads “encouraging” me to privately bank my baby’s cord blood. I put “encourage” in quotation marks because it really could be “frighten,” “scare,” “guilt,” or any number of other words that capture the marketing campaigns that target expectant parents’ fears to motivate them to spend exorbitant amounts of money to privately bank cord blood.
Before I get into the hard science that led Mac and I to decide to donate Mabel’s cord blood when she was born, and to do it again for Nemo, let me share with you a telling, albeit anecdotal fact. Of all of my friends in the sciences and medical fields, I don’t know a single one of them that paid to privately bank their children’s cord blood. However, I know many who donated the cord blood to a public bank, free of charge, and available to anyone in need of a transplant.
I think that anecdote says a lot about how convincing the science is behind cord blood banking/donation. So, how did Mac and I come to the decision to donate, rather than privately bank, our children’s cord blood? I’ll explain below, with a bit of the science background that helped us.
So, first, what is cord blood? Cord blood is basically a baby’s blood that is still in the umbilical cord and placenta after birth. The placenta is an organ grown by the extra-embryonic tissue, it’s job is to grow into the lining of the uterus and get close enough to the maternal blood supply to exchange oxygen and nutrients between mother and baby. The placenta is connected to the baby via the umbilical cord which connects right into the baby’s circulatory system. Hence, the blood in the placenta and umbilical cord is the same as that circulating in the baby. After the baby is born, there is still some blood circulating in the cord and placenta. After the cord is clamped and cut, the doctor or nurse can collect the blood remaining in the cord/placenta- that is the cord blood.
Why is it worth saving? Cord blood is rich in hematopoietic stem cells (abbreviated as HSCs), the cells responsible for forming all the types of cells found in the blood (including cells of the immune system). You may have heard of bone marrow transplants, where the HSCs are isolated from a donor’s bone marrow. While those transplants are still being performed and are beneficial, there is mounting evidence that HSCs from cord blood are better than those from adult bone marrow in several ways.
One benefit is reduced incidence of Graft-versus-host Disease (GVHD), a condition where the donor-derived cells (“graft”) recognize the cells of the recipient of the transplant (“host”) as foreign and attack them. Another benefit is that for HSCs from cord blood, the donor and recipient do not have to match their HLA types as closely as they would have to for HSCs from bone marrow. The HLA system is how our immune system tells our own cells from foreign cells, thus for an HSC transplant, the closer the donor and recipient match, the better, so the new donor cells do not consider the host cells foreign and attack them (causing GVHD). Thus, it is easier to find a suitable match from a cord blood donor than a bone marrow donor because cord blood HSCs require less HLA compatibility. (Source) For a more extensive comparison of bone marrow versus cord blood as a source of HSCs, see here.
What can it be used for? Cord blood is most often used for treating malignancies of the blood (leukemia and lymphoma for example) as well as blood disorders like certain forms of anemia and certain immunodeficiencies and metabolic disorders. (Note that none of these diseases could be treated with a child’s own cord blood because that blood would harbor the same problems.) To see a list of diseases treated with donations to the Natrional Cord Blood Program (with numbers of patients treated in each case), click here.
Many private banks will mention other, much more experimental treatments such as Diabetes and neurological disorders like cerebral palsy and brain injury. Note that these diseases are a VERY long way from being effectively and widely treated with cord blood. It is also worth mentioning that ALL treatments with cord blood are considered experimental. Read here about the National Cord Blood Program and how they supply donated cord blood under an Investigative New Drug (IND) exemption from the FDA here.
What are the disadvantages/risks of donating cord blood? The only risk my doctor mentioned, and that I can think of or find in the literature is that of NOT prolonging the delay of cord clamping. Delayed cord clamping means waiting until the umbilical cord stops pulsing before clamping and cutting the cord- this allows blood from the placenta to circulate back into the infant instead of being trapped in the placenta by the clamp. There has been a lot of research on this topic, unrelated to cord blood donation, particularly in high-risk deliveries (ie low birth weight or premature infants). Those studies do show benefits to the baby of delaying clamping, see here. While clamping early may increase the chances of collecting sufficient amounts of cord blood for donation, delaying clamping does not preclude collection of sufficient cord blood. No matter how long you delay clamping the cord, there will be blood left in the placenta/umbilical cord. I cannot find any direct links or info on the American Academy of Pediatrics’ or the American Congress of Obstetricians and Gynecologists’ (ACOG) positions on cord clamping. From secondary sources I have read, the World Health Organization does recommend delaying cord clamping until the cord stops pulsing. However, ACOG does state, in their position paper on cord blood donation, that “the collection should not alter routine practice for the timing of umbilical cord clamping.” As I said earlier, delaying clamping does not preclude collection or donation of cord blood, although it may decrease the amount of blood collected.
The only other ‘risk’ I can think of is that some blood has to be drawn from the mother to test for various blood-borne diseases. Since this is the same blood draw that most moms will have had with every prenatal screening, the risk is minimal to non-existant.
I think that this is an area that the opinion and expertise of one’s own care provider is paramount. Talk with your doctor/midwife about how he/she collects cord blood and about delaying cord clamping to find out if it is possible to donate without risk to your new baby.
Why donate to a public bank? Since I am not an MD, a pediatrician, or an obstetrician, I rely upon those who are for guidance. So, I turned to the American Academy of Pediatrics and sought their position on cord blood donation.
The American Academy of Pediatrics stated their recomendations on cord blood banking as such (emphasis mine):
1. Cord blood donation should be discouraged when cord blood stored in a bank is to be directed for later personal or family use, because most conditions that might be helped by cord blood stem cells already exist in the infant’s cord blood (ie, premalignant changes in stem cells). Physicians should be aware of the unsubstantiated claims of private cord blood banks made to future parents that promise to insure infants or family members against serious illnesses in the future by use of the stem cells contained in cord blood. Although not standard of care, directed cord blood banking should be encouraged when there is knowledge of a full sibling in the family with a medical condition (malignant or genetic) that could potentially benefit from cord blood transplantation.
2. Cord blood donation should be encouraged when the cord blood is stored in a bank for public use. Parents should recognize that genetic (eg, chromosomal ab- normalities) and infectious disease testing is performed on the cord blood and that if abnormalities are identified, they will be notified. Parents should also be informed that the cord blood banked in a public program may not be accessible for future private use.
3. Because there are no scientific data at the present time to support autologous cord blood banking and given the difficulty of making an accurate estimate of the need for autologous transplantation and the ready availability of allogeneic transplantation, private storage of cord blood as “biological insurance” should be discouraged.
Source: Cord Blood Banking for Potential Future Transplantation by the American Academy of Pediatrics
I think it’s pretty clear from the statement above. The AAP is in favor of public banking and thinks the marketing tactic of “biological insurance” is bunk. Since neither Mac nor myself, and thus Mabel, have any family history of any disorders that can currently be treated with cord blood, there was no need to privately bank. We understood that if Mabel were to develop a condition that required a HSC transplant, her own cord blood would be of no use. Further, cord blood is extremely valuable, it would be a shame to discard cord blood that could save someone’s life. The decision to donate (rather than bank or discard) was an easy one.
How do I donate my baby’s cord blood? There are two possibilities. The first, and easiest, is that your hospital is part of the National Marrow Donor Program Network. You can find out by clicking here and seeing if your hospital is listed. The second, which is still pretty easy (and certainly worth the modicum of effort to potentially save a life) is by using a cord blood bank that is associated with the National Marrow Donor Program. You can find a list of those banks here.
With Mabel’s birth, and again now with Nemo’s, neither hospital had a cord blood banking program. Thus I was left with option #2 above- using a cord blood bank associated with the National Marrow Donor Program. The bank I used was Lifeforce Cryobanks. They provide both private and public banking. I opted, for reasons mentioned above for donation to the public bank. In the following paragraphs, I’ll share my experience with you. (Note: I am not affiliated with Lifeforce Cryobanks in any way, other than having donated through them, and am not being compensated for writing this in any way. Just in case you were wondering.)
The first step was to find out if I met the minimum requirements to donate listed here. It’s important to note that you have to start the process BEFORE 32 weeks gestation so there is sufficient time to do the paperwork and get the collection kit in the mail before you deliver.
Since I met those requirements, I filled out the paperwork with all kinds of medical history info for my baby (meaning both my family history and my husband’s), had my provider (a midwife for Mabel, and OB now with Nemo) read over the info, discuss the pros/cons, and sign the forms agreeing to collect the samples and be trained on how to do so if necessary. I also double checked with them that they wouldn’t charge me for collecting the blood- and as seems to be general policy, providers do not charge for collecting if the blood is going to be donated to a public bank.
I popped those forms in the mail, and about a week later I got a phone call letting me know that I was eligible to donate, clarifying a few points, offering to answer any questions, go over the donation process, etc.
A few weeks later I received the collection kit and all the instructions in the mail. I put that in my ‘hospital go bag’ so that I would have it with me.
With Mabel, she was a scheduled induction (since she was 2 weeks late) and when we arrived we were easily able to discuss the donation with the midwife on duty as well as the nurses. We got the collection kit out, and they were ready to go.
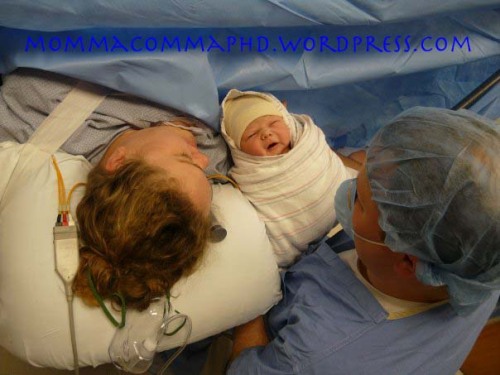
What we were doing while Mabel's cord blood was being collected: "Meet" for the first time in the OR.
Thirty-six hours later, Mabel was delivered by C-section. The staff had made sure that the collection kit accompanied me to the operating room and they collected her cord blood shortly after she was born. Later, in the recovery room, a nurse drew some blood from me to include in the kit for necessary testing.
Lifeforce Cryobanks did inform me that if I went into labor after 3pm on a Friday or before 3pm on a Sunday they wouldn’t be able to process my donation. However, I was induced on a Wednesday afternoon and Mabel finally arrived at 12:08 am on Friday. While they couldn’t/didn’t send a courier for my donation (which may be because I didn’t notify them when I went into labor/began the induction- as they now request you do), Mac was able to communicate with them to have my donation shipped out via FedEx right from the hospital’s on-site FedEx office/drop box. Was it a bit of hassle to have Mac calling Lifeforce and taking the package to FedEx himself after 36 hours of labor support? Yeah. My husband is awesome. However, we both knew that what was in that package had the potential to save a person’s life. Isn’t a little bit of running around worth that?
As it turned out, due to an error on the part of the nurse, not enough of my blood was collected for testing, and thus Mabel’s cord blood wasn’t able to be put into the public bank. However, as a scientist, one of the things I liked about donating was that if the sample was insufficient or unacceptable for use as a donation to a patient, the cells could be used by researchers. I know how hard it is to get patient samples, I am happy to enable my fellow scientists to do their research by providing a sample. If Mabel’s cord blood couldn’t be donated to directly save a person’s life, I like knowing that it could be used to further research and thus indirectly save many patients’ lives.
In talking with Lifeforce Cryobanks since my donation with Mabel’s cord blood, they have continued to improve upon their processes for collecting the cord blood (for instance, they know request TWO vials of blood from the mom to ensure they have enough to test, they have you call when you go into labor so they can arrange for a courier, etc.). I hope this go around with Nemo’s birth that all will go smoothly and we can donate again, perhaps this time with a sample that will save a patient’s life. However, if it doesn’t work out, and he arrives between the hours of 3pm Friday and 3pm Sunday, I will at least know that we tried our best to make life-saving use of his cord blood.
So what’s the take home message? Let me be clear- cord blood (and now mesenchymal stem cells from cord blood/tissue) is NOT a panacea. Many of the disorders/diseases that cord blood banks list as being treated by cord blood are in early experimental stages and a long way from being viable treatments. Further, and this is perhaps the most crucial, if your child is diagnosed with a blood cancer (leukemia, lymphoma, etc.) he/she CANNOT receive his/her own cord blood in a transplant! This is because the mutation that caused the cancer to arise in your child will also be present in his/her cord blood. So, the most common use of cord blood, hematopoietic cell transplant (also known as a bone marrow transplant when the source of the cells is bone marrow and not cord blood) is not viable if a child is diagnosed with a hematopoietic cancer. Also, there is no guarantee that siblings will be a match- so just because you bank one child’s cord blood does not mean that any other children would be guaranteed to be able to use it.
Given that Mac and I have no family history of any disorder that is currently treatable with cord blood, we felt the best course of action was to donate to a public bank. Rather than privately store a sample of blood that there is little likelihood we could every use, we donated to a public bank with a much higher chance of finding a person who could use that sample. Just like with regular blood banks, if everyone donated, there would be little need for private cord blood banking. If public cord blood banks had sufficient donations, when a person was in need of a transplant, they could turn to the public bank for it- much like we do for regular blood products.
Hope this helped! I hope this science and this perspective helps you in your decision making process on cord blood donation. Below are a bunch of links to reputable sources of information on cord blood and cord blood banking/donation. As always, your most valuable resource is your prenatal care provider, so be sure to include him/her in your decision making process.
Useful, reliable sources of info:
The National Marrow Donor Program: here.
How to publically donate with LifeForce Cryobanks: here.
How to find out if your hospital is part of the National Marrow Donor Program: here.
How to find a public cord blood bank if your hospital is not part of the National Marrow Donor Program: here.
American Congress of Obstetricians and Gynecologists position on cord blood banking/donation: here and here.
American Academy of Pediatrics position on cord blood banking/donation: here.










